- Home
- »
- Medical Devices
- »
-
Healthcare Payer Services Market Size & Share Report, 2030GVR Report cover
![Healthcare Payer Services Market Size, Share & Trends Report]()
Healthcare Payer Services Market Size, Share & Trends Analysis Report By Services (BPO Services, ITO Services, KPO Services), By Application (Claims Management Services), By End-use (Private Payers, Public Payers), By Region, And Segment Forecasts, 2023 - 2030
- Report ID: GVR-4-68039-913-3
- Number of Pages: 100
- Format: Electronic (PDF)
- Historical Range: 2018 - 2021
- Industry: Healthcare
Healthcare Payer Services Market Trends
The global healthcare payer services market size was valued at USD 61.9 billion in 2022 and is anticipated to grow at a compound annual growth rate (CAGR) of 7.6% from 2023 to 2030. The outsourcing of healthcare supply chain management services to third-party service providers is known as healthcare supply chain business process outsourcing (BPO). The growth of this market is attributed to the rise in the need for cost-effective operations and the growth in demand for advanced supply chain management (SCM) practices. Minimizing the overall cost of healthcare supply chain BPO services is likely to boost market growth during the forecast period. Furthermore, due to inventory management, the demand for healthcare supply chain business process outsourcing is increasing. Due to this reason, the market is expected to grow during the forecast period. Other factors responsible for the growth of the healthcare supply chain BPO market are a decrease in healthcare delivery costs, implementation of ICD-10 codes, and patent cliffs faced by pharmaceutical companies.
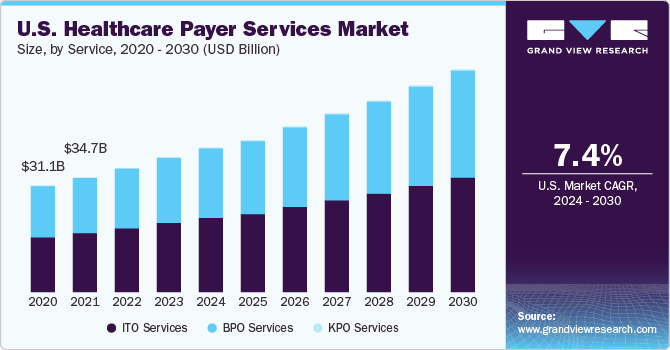
The incorporation of advanced technologies such as AI, analytics, and cloud-based service portfolios by the key players produces intense competition in the market. For example, Accenture’s cloud-based solutions diminish logistics costs, improve service revenue, and increase the availability of services for the healthcare supply chain. Hence, due to this reason, the market is expected to grow at a considerable rate. Technological advancement and integration of outsourcing processes with SCM are expected to remain the key drivers for the market during the forecast period.
The COVID-19 pandemic created challenges for healthcare payers. The reduction in healthcare funding resulted in improved financial performance for many health insurers during the pandemic. The payers supported healthcare providers vigorously. They created web portals that provide rapid and accurate information about the pandemic, expanded eligibility so that patients can retain health services, provided advance payments, and set up several community programs for health equity. For future initiatives, the key players are involved in strategic partnerships, addressing systematic health inequities.
Service Insights
The ITO services segment dominated the healthcare payer services market in terms of revenue share in 2022. The major growth factors are increasing demand for innovative and advanced technologies, a rise in investment in AI technology, information that can be easily accessed, and a rise in involvement in healthcare decisions.
However, the healthcare payer KPO segment is expected to grow at the fastest CAGR over the forecast period due to the upsurge in the demand for highly skilled professionals, and the cost advantage associated with outsourcing the high-end processes at a low cost to the developing countries. Moreover, the growing need in emerging economies for low-cost highly skilled professionals for domain-specific core and non-core activities of the payer vertical is one of the crucial factors anticipated to propel the sector growth in the coming years.
End-use Insights
The private payers segment accounted for the majority revenue share of 52.1% in 2022. This is due to the increasing private investment in the healthcare payer vertical and growing government support to promote private investment in the healthcare industry. However, the public payers segment is expected to emerge as the fastest growing with a CAGR of 9.0% during the forecast period. The increasing presence of international health insurance acts such as ACA, HIPAA, and ICD-10, growing healthcare expenditure, and rapidly decreasing out-of-pocket expenditure are some of the pivotal factors expected to positively reinforce the sector growth during the forecast period.
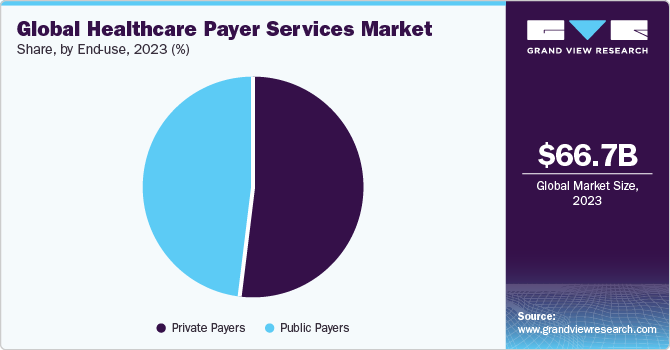
Application Insights
The claims management services segment held the majority of the market share in 2022. The presence of ACA and increasing overall healthcare expenditure are among some crucial factors that are driving the number of members enrolled in the Centers for Medicare and Medicaid Services. Claims processing services are the most data-intensive processes and form the bulk of the payer workload. The claims sent by the providers are screened for eligibility criteria, authenticity, and the exact amount that needs to be reimbursed. Due to the advent of the digital era, the procedure has been streamlined and turnaround times have improved significantly.
The analytics and fraud management services segment is expected to grow at the highest CAGR over the forecast period. The growing demand for predictive modeling and claim analytics is one of the main factors that is expected to drive the segment in the coming years. The increasing demand for low-cost skilled professionals in the developed economies to share the workload and to cater to high-end healthcare payer analytical applications, and the growing outsourcing of infrastructural management, application management, and data architecture are expected to positively reinforce this segment’s growth during the forecast period.
Regional Insights
North America dominated the market and captured a revenue share of 76.0% in 2022. The growing demand for healthcare IT services is predicted to stimulate the healthcare supply chain business process outsourcing market growth during the forecast period. Changes in regulatory scenarios and increasing pressure on the healthcare industries to decrease service costs are likely to increase the demand for healthcare supply chain business process outsourcing. Hence, the regional market is expected to witness significant growth during the forecast period.
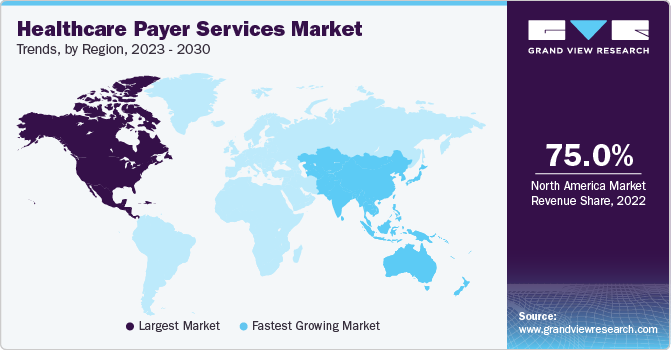
Asia Pacific is expected to advance at the fastest CAGR of 9.5% during the forecast period. This expected growth is due to rising healthcare expenditure, increasing prevalence of chronic diseases, and rising demand for resources in developing countries, like China and India. Countries such as the Philippines, China, Singapore, India, and Vietnam are at the epicenter of establishing delivery centers by the BPO service providers, thus promising higher activity from these regions during the forecast period.
Key Companies & Market Share Insights
Some key players include Cognizant, EXL, HGS Ltd., Accenture, and Genpact. Companies are focusing on research and development to introduce technologically advanced products and gain a competitive edge. Companies are also engaging in partnerships, mergers, and acquisitions, aiming to strengthen their product portfolio, and manufacturing capacities, and provide competitive differentiation. For instance, in April 2023, Cognizant, a provider of IT services, announced the extension of long-standing partnership with Microsoft in the field of healthcare. Under this partnership, healthcare payers and providers will have quick access to cutting-edge technological solutions, simplified claims processing, and improved interoperability, all of which are likely to help them improve business processes and provide better patient and member experiences.
In December 2022, Ernst & Young LLP (EY US) and EXL, a major provider of data analytics and digital operations and solutions, formed a partnership to jointly create and carry out digital transformation efforts in the insurance, financial services, and healthcare sectors, according to the EY organization.
In October 2021, HCL Technologies and Google Cloud expanded their strategic alliance to offer solutions for the healthcare and life sciences industries. The cloud-native HCL Software Platforms Digital Experience and Unica Marketing were to be combined with Google Cloud to create a joint center of excellence for Google Cloud. Payers, providers, Medtech businesses, and biopharmaceutical companies are likely to gain from this collaboration.
In addition, in August 2020, Holy Cross Health, Memorial Healthcare System, and Oscar collaborated to provide the Medicare Advantage plan; this provides virtual, affordable care provided by a trusted doctor and a connected care team.
Key Healthcare Payer Services Companies:
- Cognizant
- EXL
- HGS Ltd. (Hinduja Global Solutions Limited)
- Accenture
- Xerox Corporation
- Concentric Corporation
- Genpact
- WIPRO Ltd.
- HCL Technologies
Healthcare Payer Services Market Report Scope
Report Attribute
Details
Market size value in 2023
USD 67.0 billion
Revenue forecast in 2030
USD 111.9 billion
Growth rate
CAGR of 7.6% from 2023 to 2030
Base year for estimation
2022
Historical data
2018 - 2021
Forecast period
2023 - 2030
Quantitative units
Revenue in USD billion and CAGR from 2023 to 2030
Report coverage
Revenue forecast, company ranking, competitive landscape, growth factors, and trends
Segments covered
Service, application, end-use, region
Regional scope
North America; Europe; Asia Pacific; Latin America; MEA
Country scope
U.S.; Canada; UK; Germany; France; Italy; Spain; Denmark; Sweden; Norway; China; Japan; India; Australia; South Korea; Thailand; Brazil; Mexico; Argentina; Saudi Arabia; South Africa; UAE; Kuwait
Key companies profiled
Cognizant; EXL; HGS Ltd.; Accenture; Xerox Corporation; Concentric Corporation; Genpact; WIPRO Ltd.; HCL Technologies
Customization scope
Free report customization (equivalent up to 8 analyst’s working days) with purchase. Addition or alteration to country, regional & segment scope
Pricing and purchase options
Avail customized purchase options to meet your exact research needs. Explore purchase options
Global Healthcare Payer Services Market Report Segmentation
This report forecasts revenue growth at global, regional, and country levels and provides an analysis of the latest industry trends in each of the sub-segments from 2018 to 2030. For this study, Grand View Research has segmented the global healthcare payer services market report based on services, application, end use, and region:

-
Services Outlook (Revenue, USD Billion, 2018 - 2030)
-
BPO Services
-
ITO Services
-
KPO Services
-
-
Application Outlook (Revenue, USD Billion, 2018 - 2030)
-
Claims Management Services
-
Integrated Front Office Service and Back Office Operations
-
Member Management Services
-
Provider Management Services
-
Billing and Accounts Management Services
-
Analytics and Fraud Management Services
-
HR Services
-
-
End-use Outlook (Revenue, USD Billion, 2018 - 2030)
-
Private Payers
-
Public Payers
-
-
Regional Outlook (Revenue, USD Billion, 2018 - 2030)
-
North America
-
U.S.
-
Canada
-
-
Europe
-
UK
-
Germany
-
France
-
Italy
-
Spain
-
Sweden
-
Norway
-
Denmark
-
-
Asia Pacific
-
Japan
-
China
-
India
-
Australia
-
Thailand
-
South Korea
-
-
Latin America
-
Brazil
-
Mexico
-
Argentina
-
-
Middle East and Africa
-
Saudi Arabia
-
South Africa
-
UAE
-
Kuwait
-
-
Frequently Asked Questions About This Report
b. The global healthcare payer services market size was estimated at USD 61.9 billion in 2022 and is expected to reach USD 67.0 billion in 2023.
b. The global healthcare payer services market is expected to grow at a compound annual growth rate of 7.6% from 2023 to 2030 to reach USD 111.9 billion by 2030.
b. North America dominated the healthcare payer services market with a share of 75.9% in 2022. The key factors attributed to the majority shares include increasing investment in the healthcare payer market, the presence of a favorable reimbursement framework, and government policies such as HIPAA and HIMSS
b. Some key players operating in the healthcare payer services market include United HealthCare Services, Inc., Anthem, Inc., Aetna, Inc., Accenture, Cognizant, Xerox Corporation, and Genpact
b. Key factors that are driving the healthcare payer services market growth include increasing demand for streamlined business processes to provide better customer services and reduce the overall operating cost. Increasing use of advanced technology to drive speed and quality of healthcare payer services.
Share this report with your colleague or friend.
![gvr icn]()
NEED A CUSTOM REPORT?
We can customize every report - free of charge - including purchasing stand-alone sections or country-level reports, as well as offer affordable discounts for start-ups & universities. Contact us now
![ESOMAR Certified Member]()
![Great Place to Work Certified]()
ESOMAR & Great Work to Place Certified
![ISO 9001:2015 & 27001:2022 Certified]()
ISO 9001:2015 & 27001:2022 Certified
We are GDPR and CCPA compliant! Your transaction & personal information is safe and secure. For more details, please read our privacy policy.
We are committed towards customer satisfaction, and quality service.
"The quality of research they have done for us has been excellent."







